People Living with HIV Can Be Organ Donors
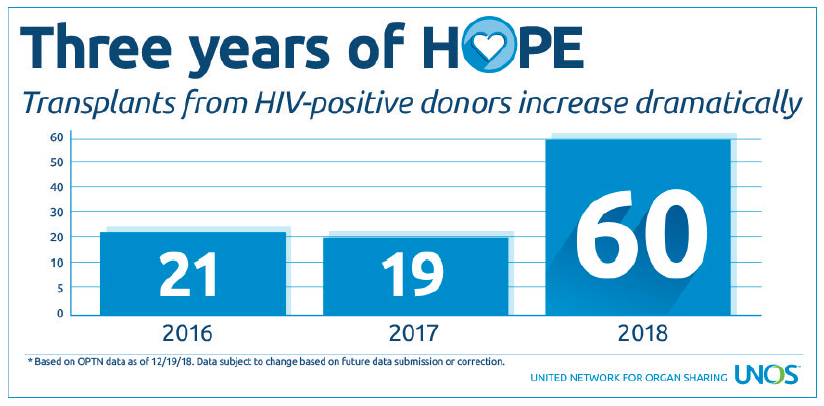
The HIV Organ Policy Equity Act (also known as the HOPE Act) provides more transplant opportunities for patients with HIV, who sometimes wait longer or are more likely to die waiting for a lifesaving organ transplant. Signed into law by President Obama in 2013, the HOPE Act authorizes the use of organs from HIV-positive donors for transplantation into HIV-positive recipients under approved research protocols. As of December 2018, 15 of the hospitals participating in HOPE Act protocols performed more than 100 successful transplants.
Know the Facts: Referring Hospitals
Timely referrals to OPOs are an important part of putting HOPE into action. Referring hospital teams should know:
- HIV is no longer an automatic rule-out for organ donation.
- Families of patients do not need to be aware of their loved one’s HIV status to be an organ donor under the HOPE Act.
- OPOs provide the same support and education to families of all potential donors, regardless of HIV status.
- Coordinating with the OPO and patient family about brain death testing or withdrawal of care is the same for potential donors, regardless of HIV status.
- It is estimated that HIV-positive donors can save up to one thousand additional lives each year. However, this can only be possible with your help and participation.
Authorization: Help for HOPE Approaches
Right now, HOPE transplants occur under a research protocol. This means that in order to draw the required blood sample, general authorization for research must be obtained as stipulated by the federal research guidelines. Research authorization can be a blanket “yes” and does not imply that the family should be informed of HIV status. This blood sample will be stored and, over time, used to test against the transplant recipient’s blood as a part of ongoing recipient follow-up specific to HIV.
It is important to note that the HOPE Act is not considered donor intervention research, meaning that HIV-negative organs are recovered in the same manner as other organs for transplant.
For more information and resources, please access the HOPE In Action Toolkit.
The content of this issue is based on a webinar presentation by Peter Stock, MD, PhD (Professor of Surgery, UCSF Medical Center, San Francisco, CA), Phil Brown (Research Program Manager, Donor Network West, San Ramon, CA), and Brianna Doby (Consultant/OPO Community, Johns Hopkins University, Baltimore, MD). A special thanks to Dr. Stock, Phil and Brianna for their contributions to this in-service. We’d also like to extend a sincere thanks to Christine Durand, MD (Co-Director, HIV Cure SWG, Johns Hopkins University) for her contributions to this educational offering.