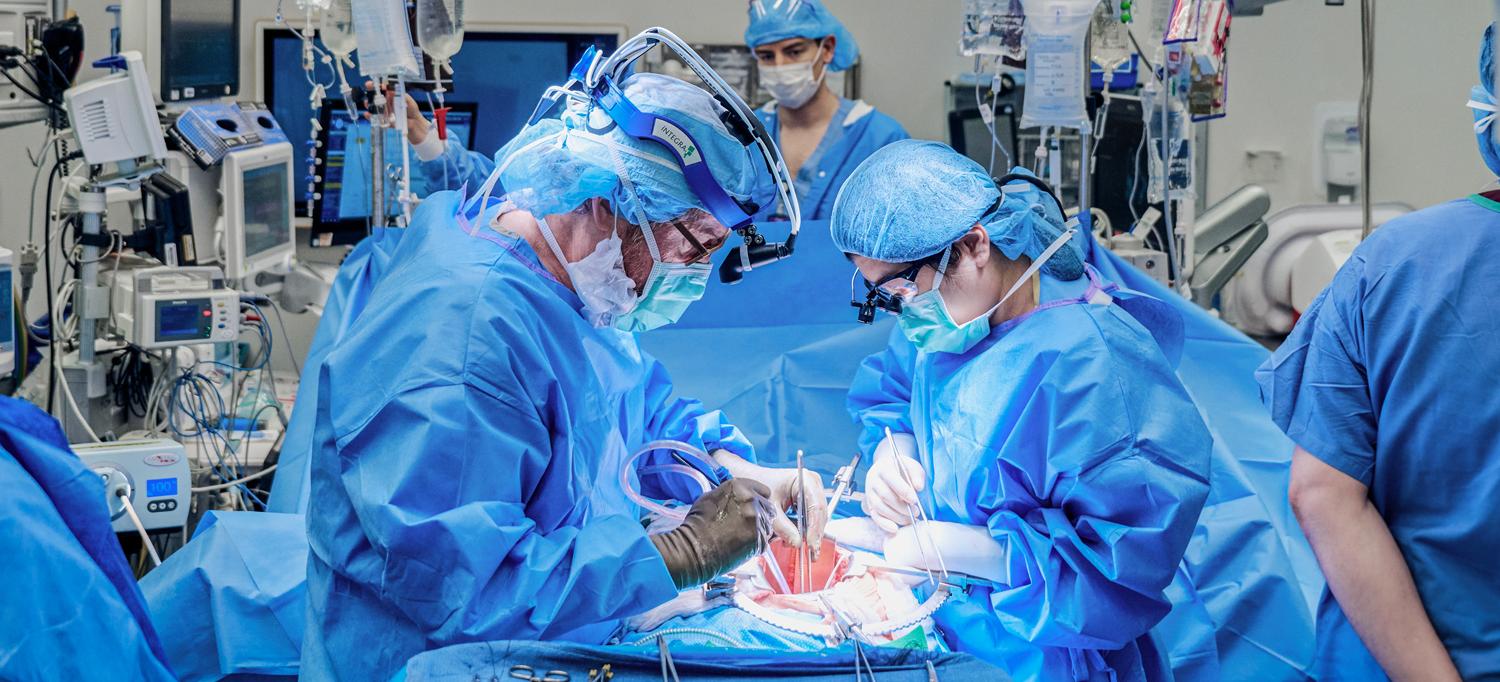
Shared from the National Academies of Sciences, Engineering, and Medicine — A new report from the National Academies of Sciences, Engineering, and Medicine finds the U.S. organ transplant system to be demonstrably inequitable; significant nonuse of donated organs — approximately 1 in 5 kidneys from deceased donors are not used; and unexplained variation in performance across the system. The report makes recommendations to address racial and other disparities, reduce nonuse of donated organs, and reduce or eliminate variations in the performance of transplant centers and organ procurement organizations.
Realizing the Promise of Equity in the Organ Transplantation System makes near- and long-term recommendations to create a fairer and more equitable, transparent, cost-effective, and efficient system for deceased donor organs. In addition to organ donors and patients, the key components of the transplantation system include donor hospitals, where the deceased donor is admitted; organ procurement organizations (OPOs), which procure organs after declaration of death; transplant centers, where the recipient is taken to surgery and gets the organ transplant; and the U.S. Department of Health and Human Services (HHS), which oversees the system’s performance. The report recommends actions that HHS should take to improve coordination across the different parts of the system, and ensure they have common goals and unified policies and processes.
Near-term actions include establishing time-bound national performance goals for the organ transplantation system. HHS should aim to reach 50,000 organs transplanted annually by 2026 and reduce nonuse rates for donated kidneys to 5 percent or less (from 20 percent nonuse at present). In addition, it should set goals to increase organ donation, procurement, transplantation, and organ offer acceptance. These goals should be reviewed annually, at minimum. Congress should hold HHS accountable for achieving demonstrable equity in the transplantation system within the next five years, the report says.
“Organ transplants depend on the generosity of individuals and their families, who are often making the decision to donate an organ to someone they have never met. The public’s trust is fundamental to the success of that system,” said Kenneth W. Kizer, chief health care transformation officer and senior executive vice president of Atlas Research and chair of the committee that wrote the report. “This report lays out a vision for an organ transplantation system that is fair and transparent, more patient- and family-centered, more accountable for performance, and better equipped to save more lives in the most equitable way.”
In the U.S., more than 110,000 patients are on the national transplant waitlist, and each day at least 17 die waiting for an organ transplant, the report says. People of color and people with disabilities are particularly disadvantaged in receiving a transplant, in referrals for transplants, and the time they spend on the waiting list. For example, Black Americans are 3 times more likely to suffer from kidney failure than white Americans, but they are substantially less likely to be placed on transplant waitlists or ultimately get an organ transplant.
Within 12 months, HHS should eliminate race from clinical equations used in allocating organs, the report recommends. Race-based thresholds for estimating kidney function can underestimate disease severity in Black patients, leaving them less likely to get needed specialty care or be placed on transplant waitlists in a timely manner. The report also considered geographic disparities. Since deceased donor organs are a national resource, the fairest way to allocate them to patients on the waiting list is on a national, continuous basis, rather than by regional geographic location, the report concludes.
Around 84 percent of patients on the national transplant list are waiting for a kidney transplantation, the report says, and many are required to undergo dialysis until a kidney is available. The Organ Procurement and Transplantation Network (OPTN), which oversees all organ transplants in the U.S., should discontinue the practice of granting allocation “credits” or “points” to patients who accrue waiting list time before beginning dialysis. Early referral and listing is not possible for all patients needing kidney transplantation, especially the socio-economically disadvantaged. Instead, waiting time “points” should be based on the date the patient began dialysis. The OPTN should closely monitor any unintended consequences of removing pre-dialysis waiting time points.
To reduce the nonuse of organs, the OPTN should make it easier for organ transplant centers to say “yes” to organ offers. Since donations occur seven days a week, the OPTN should require hospitals with transplant centers to better manage surgical scheduling, so organ procurement operations and transplants can take place in a timely manner every day. Organs at high risk of nonuse should go to transplant centers that have demonstrated a history of using — and willingness to accept — medically complex organs.
The organ transplantation system must maximize the use of already available organs, while also expanding the donor pool, the report says. It should prioritize the use of medically complex organs, including donation of organs after circulatory determination of death to meet the needs of those on the transplant waiting list.
HHS should also increase transparency about when and why organ offers are declined, and prioritize patient engagement in offer decisions, the report adds. In some instances, there are sound medical reasons to decline an organ offered to an individual, but patients should be made aware of this information. HHS should develop, implement, and evaluate rigorous approaches for transplant teams to communicate with potential transplant recipients about their status. Waitlisted candidates should receive information about the benefits, risks, and alternatives to accepting different types of organs to inform their decision about whether to accept an organ.
The sooner an organ can be transplanted, the better, the report emphasizes. Policies should consider ways to gradually increase the number of simultaneous offers of a given organ made to transplant centers on behalf of patients. It will be important to reduce the time between the chilling of an organ (when the organ is not receiving a blood supply) to the time it is transplanted into the recipient. HHS should also require all of the nation’s 57 OPOs to create, establish, and manage a donor care unit. Donor care facilities provide dedicated space for deceased donors and their families, increase cost-effectiveness in organ procurement, and allow organ procurement to take place in a dedicated surgical facility, avoiding the complications and delays of organ procurement in a traditional hospital setting.
There are widespread variations in practices and performance among donor hospitals, OPOs, and transplant centers, which can affect the quality of patient care, the report concludes. HHS should create a publicly available dashboard of standardized performance measures to identify such variations and track performance across the organ transplantation system as a whole. The metrics in the dashboard should be meaningful to patients and families, taking into account patient referral for transplant evaluation, time on the waiting list, and post-transplant quality of life.
The study — undertaken by the Committee on a Fairer and More Equitable, Cost-Effective, and Transparent System of Donor Organ Procurement, Allocation, and Distribution — was sponsored by the National Institutes of Health. The National Academies of Sciences, Engineering, and Medicine are private, nonprofit institutions that provide independent, objective analysis and advice to the nation to solve complex problems and inform public policy decisions related to science, technology, and medicine. They operate under an 1863 congressional charter to the National Academy of Sciences, signed by President Lincoln.