The recent report from the National Academies of Sciences, Engineering, and Medicine (NASEM), outlined several recommendations for OPOs and Transplant Centers for consideration to eliminate variations in performance measures and reduce the nonuse of donated organs. Establishment of one or more Donor Care Units (“DCU”) within each OPO service area is one of those recommendations that could have a significant impact on caring for donor families, honoring the gift of donation and saving more lives. 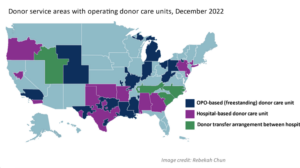
Many OPOs have embraced the guidance received from the NASEM report by instituting a variety of DCU models and the Fall 2022 issue of the Alliance Hospital Executive Insights entitled: Maximizing the Gift with a Donor Care Unit: A Hospital-Based Approach explored the hospital based model. Another best practice option is the OPO based model, which represents about 50% of all DCU models among OPOs.
Why Implement an OPO based DCU?
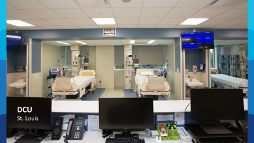
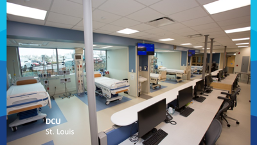
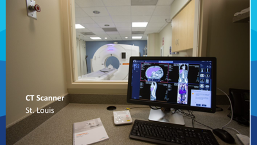
The impetus to consider an alternative location for organ procurement arose from complaints by donor hospitals’ intensive care unit (ICU) medical directors alleging that organ donor cases were taking too long and occupying one of their scarce ICU beds. To address this challenge, an OPO based on-site DCU concept was created with Mid-America Transplant pioneering the first and Mississippi Organ Recovery Agency (MORA), along with several more OPOs following suit. This gives an OPO the ability to accommodate organ donors more quickly and place less strain on hospital partners, so their facilities could accommodate living patients. ICU nurses and a medical director, along with employees of the OPO, manage the donors and oversee hemodynamic monitoring, critical care ultrasounds and high-definition bronchoscopy, while contracted sonographers and radiology technicians conduct echocardiograms and CTs. The DCU is coupled with onsite laboratory services to provide routine chemistry, hematology, coagulation, and urine and blood gas testing. Since the inception of the OPO based DCUs, hundreds of organ donor heroes have been cared for by dedicated and passionate staff that work tirelessly to carry out their life-saving missions.
How Donor Care Units Benefit Hospitals and Increase Overall Organ Transplants
While the healthcare community is overwhelmingly aligned in its support of organ donation, the logistics of managing donors can often be at odds with the hospital’s primary mission – to provide care to living patients. More than 20 years ago, Mid-America Transplant transformed the future of donor management by creating the first-ever independent donor care unit (DCU), shifting the responsibility for donor management and recovery from the hospital to organ procurement organization (OPO) staff, and ultimately making more life-saving organ transplants possible. Since then, several other OPOs have followed suit, including Mississippi Organ Recovery Agency (MORA), who opened up their center in October, 2017.
Impact on Culture of Donation
Since this concept debuted, the independent DCU model has transformed how hospitals and OPOs work together to manage donors. Today, 24 of the 56 U.S. OPOs operate under some version of this model and have provided several important benefits for the medical community. For donor hospitals, moving a donor to a separate facility frees up an ICU bed and operating room that can be filled with a critical living patient.
Recognizing that hospital staff care closely for the donor, most OPOs invite them to participate in routines to honor and celebrate the donor such as gathering in the hallways as the donor is taken away to the DCU. OPOs also follow up afterwards to let hospital staff and leadership know which organs and tissues were able to be placed, as well as general information about the recipients.
DCUs relieve the strain on hospital resources required for the process of donor evaluation, management and organ recovery. Centralizing OPO dedicated resources to provide these services in a space that doesn’t compete for hospital resources, allows the process to move quicker, which means life-saving organs can be on their way to a transplant center sooner and ultimately, positively impact recipient outcomes.
Donor Family Conversations & Support
Donor families benefit from knowing their loved one will be cared for in a dedicated donor unit, inspiring trust and reassurance. Donor families are usually exhausted from living at the hospital for days because their loved one is cared for in the ICU. After they are informed that their loved one is dead, they are generally relieved that they can go home, make funeral arrangements, and continue the grieving process while the donor is managed at the DCU. In a DCU, we are able to honor the wishes of the family, such as playing the donor’s favorite music, or dedicating a moment before the procurement for reciting a prayer or reading a letter from the family.
Optimization Efforts
Due to centralized dedicated resources, donor management in a dedicated donor care unit is proven to be consistent and efficient. Since this model was first introduced more than 20 years ago, the OPO industry has seen significant improvements in the organ procurement process, including:
- Increased organ yield, largely due to the expertise of the DCU staff who are focused only on donor management.
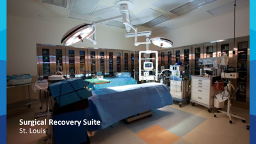
- More expeditious organ recovery process due to dedicated operating suites. This allows the accommodation of transplant programs and surgeon preferences therefore potentially increasing the number of organs recovered for transplant.
- Provides opportunities to conduct clinical research and implement processes designed to improve organ quality. For example, implementing a unique prone ventilation protocol at Mid-America Transplant’ DCU increased the number of lungs transplanted from 24% to 45%.
- Specialty roles are crucial in optimizing organ function and increasing placement opportunities, which is another important benefit of a DCU. For example, MORA hired full time critical care respiratory therapists in 2020 and adopted an aggressive prone ventilation protocol, which resulted in significant increases in lung utilization over prior years.
All of this enables OPOs to place more organs for transplant each year. In Mid-America Transplant’s case, 497 organs were transplanted in 2007 before their freestanding DCU opened. In 2022, 772 organs were placed, and much of this growth can be attributed to the benefits provided by the DCU.
The impact on the transplant side is equally beneficial as noted by Dr. Aladdein Mattar, Assistant Professor of Surgery at Baylor College of Medicine, “DCUs provide the best model for organ recovery with consistent and convenient scheduling knowing there are no hospital emergency conflicts. The harmony and dedication of the recovery team at MORA provides a great surgical environment. As a cardiothoracic surgeon, I am delighted knowing that I will be recovering at MORA. This model facilitates more organ donation and helps us to provide the best patient care.” I
Testimonials
“Because of the generous donors and their families, and due to the innovative approaches that a DCU allows, MORA has seen a 40% increase in organs transplanted since the inception of their DCC model”, states Joe Doherty, M.D., Board Certified in Emergency Medicine, Surgery, and Surgical Critical Care at The University of Mississippi Medical Center
In fact, Dr. Doherty shared that the partnership between MORA’s Donor Care Center and UMMC has been and continues to be advantageous in the process of saving and improving lives through organ donation. Dr. Doherty notes that the Donor Care Center:
- Minimizes hospital bed shortages
- Provides more focused and intense care to brain-dead patient
- Improves donor outcomes
- Alleviates the extended use of hospital staff
- Relieves ICU and ER staff responsibilities